What is ventriculomegaly?
The two components of the central nervous system are the brain and the spinal cord. The entire surface of the brain and spine cord is bathed by a fluid called cerebrospinal fluid (CSF). Cerebrospinal fluid is a clear liquid that surrounds the brain and spinal cord to provide cushioning from jolts. CSF is made in cavities in the brain called the lateral ventricles, and flows through the ventricles to surround the brain and spinal cord.
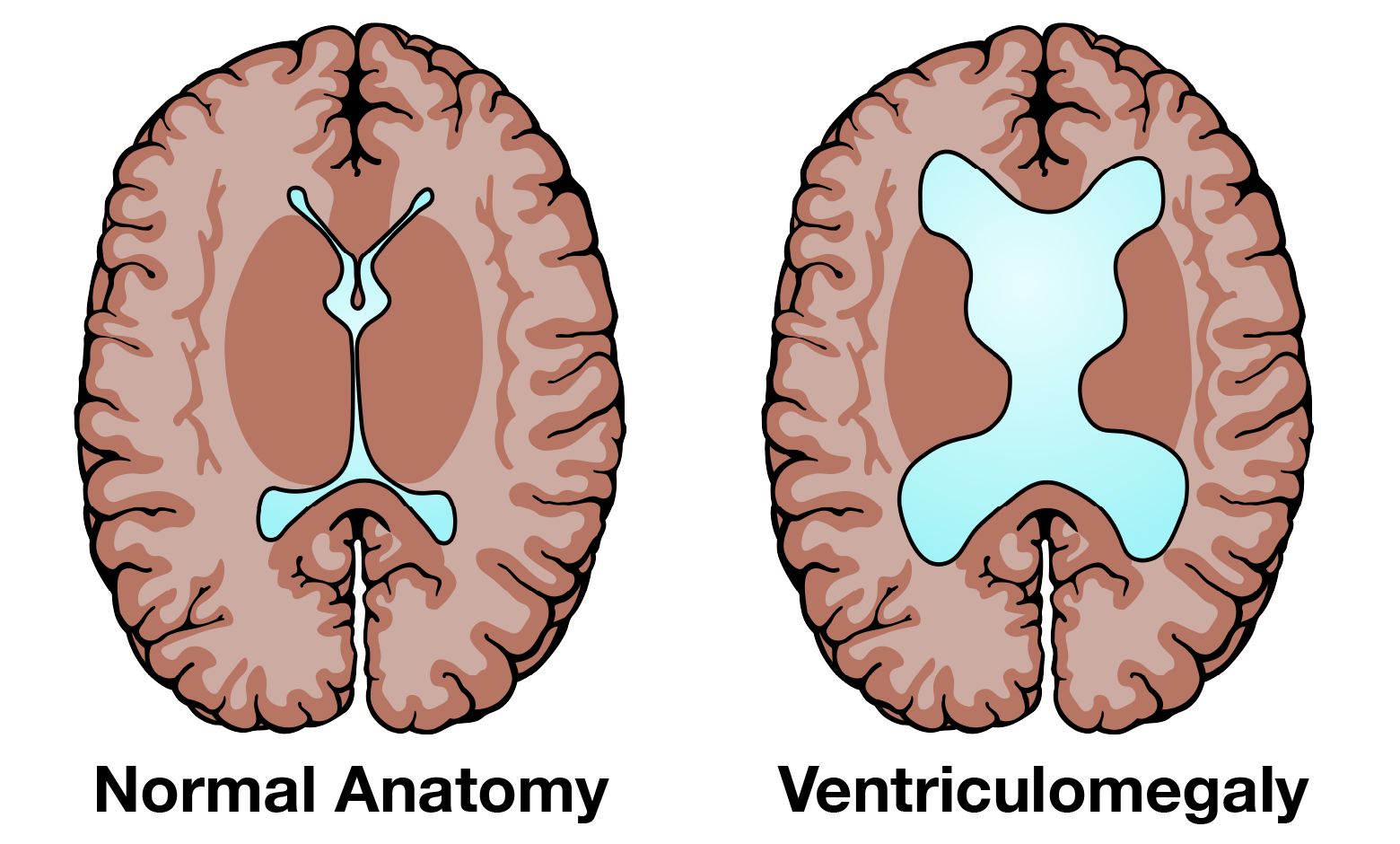
Ventriculomegaly is when the fluid filled structures in the brain are too large. When you are pregnant you will have an ultrasound. With the ultrasound the doctor will look at your fetus’s brain and measure the ventricles. If the lateral ventricles are 10 millimeters or greater in size then you will be told that your fetus has "ventriculomegaly".
Sometimes the ultrasound will only show one of the lateral ventricles even though there are two (one on the right, and one on the left side). Ventriculomegaly is slightly more common in male fetuses than in female fetuses.
What is the outcome for a fetus with ventriculomegaly?
The outcome of ventriculomegaly depends on several factors including the actual size of the ventricles, whether or not there are any other findings in the brain, such as agenesis of the corpus callosum, and the results of the amniocentesis. In general, the outcome is worse when the ventricles are larger, the amniocentesis is abnormal, or there are other problems seen on the ultrasound. The best outcome is typically observed when:
- Ventricular enlargement is not in the severe range (or measuring >15 millimeters in size)
- If there are no other problems seen in the brain
- The genetic testing results are normal—this is called Isolated Mild Ventriculomegaly
The exact outcome for your child’s health is difficult to know. The most common effect in the child is developmental delay. This seems to be related to the size of the ventricles, whether the ventriculomegaly is isolated and the cause.
How serious is my fetus’s ventriculomegaly?
If your doctor sees ventriculomegaly, they may refer you for several tests. These include a more detailed ultrasound (often times called level II ultrasound or fetal survey), amniocentesis and/or microarray (to look at the genetic makeup of your fetus, and to look for any signs of infection), and fetal magnetic resonance imaging (Fetal MRI).
Fetal MRI is another way to safely look at your fetus’s brain. It gives pictures of your fetus’s brain using different technology than ultrasound. Because it uses a different technology, fetal MRI can detect other problems in your fetus’s brain that cannot be detected on ultrasound. We can then look at the results from all of the tests together and your physician can speak with you about the significance of these test results.
For more information on Fetal MRI please visit UCSF Baby Brain - Fetal MRI
What are my choices during this pregnancy?
There is no treatment before birth for fetuses with ventriculomegaly. Treatment after birth involves managing the child's symptoms and supporting their development. It is important during your pregnancy to get a detailed diagnosis (via detailed ultrasound, amniocentesis, and MRI) in order to determine if there are any additional problems. Our staff can talk to you about these test results and inform you what challenges you may expect. If there is evidence of more severe problems which may require long-term care, we can help direct you to the appropriate specialists.
Hydrocephalus and ventriculoperitoneal shunt (VP shunt)
If tests show that your baby's cerebrospinal fluid is not draining well and the ventricles are severely enlarged, this may indicate hydrocephalus. Hydrocephalus is the buildup of cerebrospinal fluid which causes pressure on the brain. In such a situation, a ventriculoperitoneal shunt (VP shunt) may be needed. Hydrocephalus is a progressive problem so usually the fluid builds up slowly over the course of weeks after your baby is born. In most cases we will know by 6 months if your baby will need a VP shunt.
A VP shunt is the surgical implantation of a small plastic catheter that drains the cerebrospinal fluid into a part of the body that can easily absorb the fluid such as the abdomen or peritoneum (membrane that forms the lining of the abdominal cavity). The VP shunt procedure will be performed by a pediatric neurosurgeon. It is a very safe procedure which can help your child's development as it helps relieve pressure to the brain caused by the buildup of cerebrospinal fluid. Your child will not have to stay in the hospital as the shunt lives under the skin. Many children live their lives healthfully with a VP shunt. Patients with a VP shunt will require regular follow up with neurosurgery to make sure the shunt continues to function properly.
Support Groups & Other Resources
- March of Dimes — Researchers, volunteers, educators, outreach workers and advocates working together to give all babies a fighting chance
- Birth Defect Research for Children — a parent networking service that connects families who have children with the same birth defects
- Kids Health — doctor-approved health information about children from before birth through adolescence
- CDC - Birth Defects — Dept. of Health & Human Services, Centers for Disease Control and Prevention
- NIH - Office of Rare Diseases — National Inst. of Health - Office of Rare Diseases
- North American Fetal Therapy Network — NAFTNet (the North American Fetal Therapy Network) is a voluntary association of medical centers in the United States and Canada with established expertise in fetal surgery and other forms of multidisciplinary care for complex disorders of the fetus.